If you’ve ever watched a University of Florida football game on TV, you’ve probably seen a commercial for UF & Shands. They use the tag line “UF & Shands - The Science of Hope.” I used to think that just a line dreamed up by the UF administration’s marketing consultant to impress the editors of US News & World Report when it came time for the annual hospital rankings. I don’t think that anymore. In an earlier post, I mentioned Ginny’s neighbor from Baton Rouge, Louisiana. Baby Joseph and his parents Max and Deborah have changed my mind. They’ve asked me to share his story with you.
Max is 34 years old and Deborah is 27. They live just outside Baton Rouge, Louisiana and both are big LSU Tiger fans. She is a first grade teacher, and he is mechanical drafter in the petrochemical industry. They had been married just over a year and were having trouble conceiving a child, so they went to a fertility specialist. The specialist did not give them much chance of conceiving on their first try, but in September they were happy to learn they were pregnant.
In January, they went for their 20 week ultrasound to find out if their bundle of joy would be a boy or a girl. During the ultrasound the doctor kept looking at one particular area of the baby. He didn’t say anything. “Is it a boy or a girl,” they finally asked. “A boy,” the doctor replied, “but there is a problem.” They found that Joseph had a condition called Congenital Diaphragmatic Hernia (CDH). CDH is a life threatening birth defect where the diaphragm does not completely form, allowing some of the contents of the abdomen to protrude into the chest and hinder the normal growth of lung tissue. CDH affects about 1 in 3000 babies, and the national survival rate for babies born with CDH is between 50% and 65%. (www.realhopeforcdh.com)
The doctor encouraged them to “consider your options. You are only 20 weeks.” They understood that he was telling them to have an abortion. For them, that was not an option. The next day they traveled to another specialist at a university hospital in New Orleans. He gave the same prognosis. They were not given much hope. The only way their baby would survive is if he was born at a hospital with a CDH center. They were told even then he didn’t have much chance.
Max and Deborah immediately began researching hospitals with CDH centers. There are only five centers in the country that handle these kinds of cases. They first visited the University of Florida and Shands Hospital. Deborah underwent a battery of tests and then met with Dr. David Kays. Dr. Kays is an Associate Professor and Chief of Pediatric Surgery and arguably the best doctor in the country for the treatment of CDH. He met with them and explained is approach to treatment and gave them an 80 to 90% chance that Joseph would survive. Finally someone had given them a reason to be hopeful.
They also traveled to a children’s hospital in Philadelphia. The doctors there gave them a best-case chance of survival of 40% and were not very encouraging. Their decision had been made for them. Joseph would be born at Shands.
At 27 weeks, Deborah was diagnosed with polyhydraminosis – a condition where her body created too much amniotic fluid. By 33 weeks, her body had created over a gallon of excess fluid. The extra fluid could send her into pre-term labor and had to be removed by a procedure called amnio-reduction. Because of the risk of pre-term labor, and because Joseph’s chances of survival were greatly diminished if he was born before 39 weeks, Deborah and Max moved to Gainesville for the last 5 weeks of their pregnancy. During that 5 week period, Deborah experienced almost constant contractions and pain, and they made 7 or 8 trips to the emergency room thinking she was in active labor.
Joseph was delivered by Caesarian section on June 1st at 9:05 a.m. He weighed 7 pounds, 14 ounces, and was 20 ½ inches long. Immediately after his birth he was placed on the ventilator and brought to the NICU. He moved into the bed space right next to Ginny. Deborah and Max weren’t able to see him until 4:30 that afternoon.
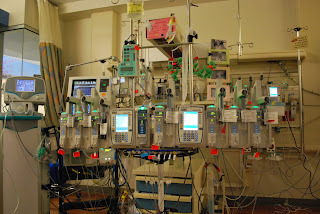
The first time you see your baby in a NICU crib - with the wires and IV’s and ventilator tubes, and the constant beeping from monitors and IV pumps – a wave of emotion crashes over you, almost to the point of physically knocking you to your knees. It is not how you envisioned meeting your child, and the feelings border on devastation. We were there when Joseph finally got to meet his parents, and it was no different for them. It is an experience I wish happened less frequently, but we have seen it several times over the last month.
On June 4th – when Joseph was just 3 days old – Dr. Kays and his team performed surgery to repair Joseph’s hernia. His diaphragm was repaired using a gore-tex fabric. Then his digestive tract had to be reconstructed – including rearranging his stomach, liver, intestines, and spleen into something resembling their normal positions. To me that sounds hard enough on a full grown man, but they did it on a 7 pound boy.
Joseph has been recovering well. On June 12th he was taken off of the ventilator and he has been moved from NICU 3 to NICU 2 – a good sign. He is feeding and should be well enough to leave the hospital in just a couple weeks. Deborah and Max have become friends of ours through our shared experience in the NICU. Ginny and Joseph are planning play-dates that coincide with the LSU vs. Florida football weekend. During that game, we won’t be so cynical about the commercials for UF & Shands.